It’s time to do the impossible. It’s time to turn the tide.
 In my last blog, I talked about the exponential potential of what could be possible if clinicians worked together in a more collaborative way. However, far more can be achieved if we work together in and with our communities to create a social movement together around being more healthy and well. I’ve talked previously about the “battle royale” that occurred between Béchamp and Pasteur over whether we should promote health or fight disease. The answer is, of course, that we need to do both, but the clinical community is not equipped with the resource or power to do it alone.
In my last blog, I talked about the exponential potential of what could be possible if clinicians worked together in a more collaborative way. However, far more can be achieved if we work together in and with our communities to create a social movement together around being more healthy and well. I’ve talked previously about the “battle royale” that occurred between Béchamp and Pasteur over whether we should promote health or fight disease. The answer is, of course, that we need to do both, but the clinical community is not equipped with the resource or power to do it alone.
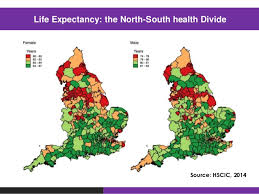
What we cannot accept, though, is our current apathy or malaise that some of the health  crises we now face are too much for us to do anything about. We are in the midst of a battle, which we are currently losing and it is time to gird our loins for a turning of the tide. Here in Morecambe Bay, we have started a conversation, not just among the Clinical Community but with the wider population about how we might become the healthiest place in the UK. Yes, we mean this in a very holistic way, but there are also some specific foci we have so we can together reverse some of the appalling health statistics we are facing.
crises we now face are too much for us to do anything about. We are in the midst of a battle, which we are currently losing and it is time to gird our loins for a turning of the tide. Here in Morecambe Bay, we have started a conversation, not just among the Clinical Community but with the wider population about how we might become the healthiest place in the UK. Yes, we mean this in a very holistic way, but there are also some specific foci we have so we can together reverse some of the appalling health statistics we are facing.
For too long, we have simply laid down and allowed exercise to be taken out of schools, whilst our kids consume a bath full of sugar every year. All the time our own work and eating habits have become significantly unhealthy. We have relied on expensive drugs to fix our problems, rather than tackling the root causes of our excesses. It has lead to 1 in every 5 pounds in the NHS being spent as a direct result of our lifestyles and 1 in 11 pounds being spent on diabetes. We say we value the NHS above anything else as a nation (maybe an issue in it’s own right…..) but we do not behave in ways that show this value to be true. We have not been brave enough to challenge the status quo and together make a wholesale change both about how we promote health and look to aggressively reverse it when things begin to go wrong.
 I suggest that within a generation, if we wanted to, we could render Type 2 Diabetes a rare diagnosis. We can do this through encouraging far more healthy lifestyles in our children and young people now, like running a mile a day and learning to eat food that doesn’t actually harm them! I believe we could significantly reduce the need for so many people to be taking medication for hypertension and diabetes now, prevent many strokes and heart attacks, by being violent towards these conditions with major changes in lifestyle, though diet and exercise, rather than the prescription of drugs, using coaching, peer support and local champions to give psychological motivation and encouragement. We are beginning to have some excellent discussions and develop some exciting plans around this.
I suggest that within a generation, if we wanted to, we could render Type 2 Diabetes a rare diagnosis. We can do this through encouraging far more healthy lifestyles in our children and young people now, like running a mile a day and learning to eat food that doesn’t actually harm them! I believe we could significantly reduce the need for so many people to be taking medication for hypertension and diabetes now, prevent many strokes and heart attacks, by being violent towards these conditions with major changes in lifestyle, though diet and exercise, rather than the prescription of drugs, using coaching, peer support and local champions to give psychological motivation and encouragement. We are beginning to have some excellent discussions and develop some exciting plans around this.
Our NHS health checks should serve as a major motivational opportunity for someone to pull themselves back from the brink of a lifetime of medication and we should use all medication reviews as a chance to help people adopt lifestyles that might reverse the need for such drugs. In the process, we would also significantly reverse our number of cancer diagnoses – many of which are linked to our lifestyle choices. We simply can’t afford for our current and failing approach to continue. We need to be braver together! And this means the NHS must be willing to partner in new ways, not only with local people, but also with businesses like the major supermarkets to help reverse our current direction towards the abyss, in which there is no longer a healthcare system that serves the needs of everyone, no matter where they come from or how much they do or don’t earn.
pull themselves back from the brink of a lifetime of medication and we should use all medication reviews as a chance to help people adopt lifestyles that might reverse the need for such drugs. In the process, we would also significantly reverse our number of cancer diagnoses – many of which are linked to our lifestyle choices. We simply can’t afford for our current and failing approach to continue. We need to be braver together! And this means the NHS must be willing to partner in new ways, not only with local people, but also with businesses like the major supermarkets to help reverse our current direction towards the abyss, in which there is no longer a healthcare system that serves the needs of everyone, no matter where they come from or how much they do or don’t earn.
Don’t get me wrong! We should absolutely use medication to its fullest use for those who are at risk and have not responded to major lifestyle changes. For example, we can wage war on Atrial Fibrillation, ensuring far more appropriate use of anticoagulation, in the most cost effective and safest way, therefore preventing many life-changing strokes in the mean time. And for those who, despite lifestyle measures, still have a high blood pressure or continue with diabetes, we should not withhold medication that would prevent major issues later on. It’s just at the moment, we’re reaching for the prescription pad too readily and not looking to reverse conditions completely before they set in. We need more education out there around the early signs of cancer, so we can hit it early and reverse it’s effects when we have a better chance. Respiratory disease is another area where we could seriously make a change. We need to think of ourselves as one big respiratory team, tackling smoking, housing damp and carpeting, whilst ensuring every person has an understanding of their condition, how to use their medication effectively and what to do when things flare up. A cohesive clinical community really could deliver something special in each of these disease areas.
We could also be a great deal more effective in how we care for the frail elderly. We don’t need anywhere near as many hospital beds. We can provide care in residential and nursing homes, avoiding double payment for beds, by shifting resource out of our acute hospitals and into the community. We need to have a far more grown up conversation about why we admit people to hospital when there is very little proven benefit of doing so.
Taking a strategic shift towards a social movement for health, significant lifestyle changes and treatment only after these things have been given serious attention, but unapologetically so once they have, we can turn back this battle at the gates and change the health of this nation for generations to come. We can undo the unaffordable situation we find ourselves in and discover together a much more healthy future.
 We can absolutely do this!! It’s going to take some serious resolve and we’re going to have to withstand the fear and pressure of some pretty powerful lobbies, like the sugar, alcohol, tobacco and pharmaceutical giants, and perhaps even the government itself, but it is time for us to do the impossible. With love, hope and faith, we can do this! Yes we need to focus on schools and work places. Yes, we need to partner with organisations we’ve never worked with before. Yes, we need a far more effective media strategy and yes, we need to allow clinicians to work very differently. But we cannot do nothing. So let’s try something a whole lot more radical. That’s what we’re going for in Morecambe Bay – not just better care together, but better health together – you can watch and wait, and see if we sink or swim, or you can join us!
We can absolutely do this!! It’s going to take some serious resolve and we’re going to have to withstand the fear and pressure of some pretty powerful lobbies, like the sugar, alcohol, tobacco and pharmaceutical giants, and perhaps even the government itself, but it is time for us to do the impossible. With love, hope and faith, we can do this! Yes we need to focus on schools and work places. Yes, we need to partner with organisations we’ve never worked with before. Yes, we need a far more effective media strategy and yes, we need to allow clinicians to work very differently. But we cannot do nothing. So let’s try something a whole lot more radical. That’s what we’re going for in Morecambe Bay – not just better care together, but better health together – you can watch and wait, and see if we sink or swim, or you can join us!




 In my last blog, I talked about the exponential potential of what could be possible if clinicians worked together in a more collaborative way. However, far more can be achieved if we work together in and with our communities to create a social movement together around being more healthy and well. I’ve talked previously about the “battle royale” that occurred between Béchamp and Pasteur over whether we should promote health or fight disease. The answer is, of course, that we need to do both, but the clinical community is not equipped with the resource or power to do it alone.
In my last blog, I talked about the exponential potential of what could be possible if clinicians worked together in a more collaborative way. However, far more can be achieved if we work together in and with our communities to create a social movement together around being more healthy and well. I’ve talked previously about the “battle royale” that occurred between Béchamp and Pasteur over whether we should promote health or fight disease. The answer is, of course, that we need to do both, but the clinical community is not equipped with the resource or power to do it alone. crises we now face are too much for us to do anything about. We are in the midst of a battle, which we are currently losing and it is time to gird our loins for a turning of the tide. Here in Morecambe Bay, we have started a conversation, not just among the Clinical Community but with the wider population about how we might become the healthiest place in the UK. Yes, we mean this in a very holistic way, but there are also some specific foci we have so we can together reverse some of the appalling health statistics we are facing.
crises we now face are too much for us to do anything about. We are in the midst of a battle, which we are currently losing and it is time to gird our loins for a turning of the tide. Here in Morecambe Bay, we have started a conversation, not just among the Clinical Community but with the wider population about how we might become the healthiest place in the UK. Yes, we mean this in a very holistic way, but there are also some specific foci we have so we can together reverse some of the appalling health statistics we are facing. I suggest that within a generation, if we wanted to, we could render Type 2 Diabetes a rare diagnosis. We can do this through encouraging far more healthy lifestyles in our children and young people now, like running a mile a day and learning to eat food that doesn’t actually harm them! I believe we could significantly reduce the need for so many people to be taking medication for hypertension and diabetes now, prevent many strokes and heart attacks, by being violent towards these conditions with major changes in lifestyle, though diet and exercise, rather than the prescription of drugs, using coaching, peer support and local champions to give psychological motivation and encouragement. We are beginning to have some excellent discussions and develop some exciting plans around this.
I suggest that within a generation, if we wanted to, we could render Type 2 Diabetes a rare diagnosis. We can do this through encouraging far more healthy lifestyles in our children and young people now, like running a mile a day and learning to eat food that doesn’t actually harm them! I believe we could significantly reduce the need for so many people to be taking medication for hypertension and diabetes now, prevent many strokes and heart attacks, by being violent towards these conditions with major changes in lifestyle, though diet and exercise, rather than the prescription of drugs, using coaching, peer support and local champions to give psychological motivation and encouragement. We are beginning to have some excellent discussions and develop some exciting plans around this. pull themselves back from the brink of a lifetime of medication and we should use all medication reviews as a chance to help people adopt lifestyles that might reverse the need for such drugs. In the process, we would also significantly reverse our number of cancer diagnoses – many of which are linked to our lifestyle choices. We simply can’t afford for our current and failing approach to continue. We need to be braver together! And this means the NHS must be willing to partner in new ways, not only with local people, but also with businesses like the major supermarkets to help reverse our current direction towards the abyss, in which there is no longer a healthcare system that serves the needs of everyone, no matter where they come from or how much they do or don’t earn.
pull themselves back from the brink of a lifetime of medication and we should use all medication reviews as a chance to help people adopt lifestyles that might reverse the need for such drugs. In the process, we would also significantly reverse our number of cancer diagnoses – many of which are linked to our lifestyle choices. We simply can’t afford for our current and failing approach to continue. We need to be braver together! And this means the NHS must be willing to partner in new ways, not only with local people, but also with businesses like the major supermarkets to help reverse our current direction towards the abyss, in which there is no longer a healthcare system that serves the needs of everyone, no matter where they come from or how much they do or don’t earn. We can absolutely do this!! It’s going to take some serious resolve and we’re going to have to withstand the fear and pressure of some pretty powerful lobbies, like the sugar, alcohol, tobacco and pharmaceutical giants, and perhaps even the government itself, but it is time for us to do the impossible. With love, hope and faith, we can do this! Yes we need to focus on schools and work places. Yes, we need to partner with organisations we’ve never worked with before. Yes, we need a far more effective media strategy and yes, we need to allow clinicians to work very differently. But we cannot do nothing. So let’s try something a whole lot more radical. That’s what we’re going for in Morecambe Bay – not just better care together, but better health together – you can watch and wait, and see if we sink or swim, or you can join us!
We can absolutely do this!! It’s going to take some serious resolve and we’re going to have to withstand the fear and pressure of some pretty powerful lobbies, like the sugar, alcohol, tobacco and pharmaceutical giants, and perhaps even the government itself, but it is time for us to do the impossible. With love, hope and faith, we can do this! Yes we need to focus on schools and work places. Yes, we need to partner with organisations we’ve never worked with before. Yes, we need a far more effective media strategy and yes, we need to allow clinicians to work very differently. But we cannot do nothing. So let’s try something a whole lot more radical. That’s what we’re going for in Morecambe Bay – not just better care together, but better health together – you can watch and wait, and see if we sink or swim, or you can join us! We need to reimagine ourselves as all being part of a team who are together tackling the health crises we are facing. We know only too well that, as just one example among many, we are failing kids with asthma because we have not joined up our resources or thinking adequately enough. Yes there are major issues with housing, smoking and pollution, but let’s not point the finger or push the problem somewhere else. Let’s use the phenomenal brains God has given us to pull the right people round the table and work out what we’re going to do about it. Let’s change the way we spend our time so that we’re in schools, we’re listening to our communities and we’re partnering together outside of our normal comfort zones to change the health of the generations to come. We know only too well, that if we don’t shift our focus towards population health and work more intentionally with our communities, doing things with them rather than too them, we will never win this battle. We’re not about playing political games. We are about working with our communities to create optimal health for every person no matter who they are or where they are from. We need to be braver, push the boat away from the shore we know and face the uncertain waters of working altogether differently. In my next blog I will explore some of the possible ways we could work differently.
We need to reimagine ourselves as all being part of a team who are together tackling the health crises we are facing. We know only too well that, as just one example among many, we are failing kids with asthma because we have not joined up our resources or thinking adequately enough. Yes there are major issues with housing, smoking and pollution, but let’s not point the finger or push the problem somewhere else. Let’s use the phenomenal brains God has given us to pull the right people round the table and work out what we’re going to do about it. Let’s change the way we spend our time so that we’re in schools, we’re listening to our communities and we’re partnering together outside of our normal comfort zones to change the health of the generations to come. We know only too well, that if we don’t shift our focus towards population health and work more intentionally with our communities, doing things with them rather than too them, we will never win this battle. We’re not about playing political games. We are about working with our communities to create optimal health for every person no matter who they are or where they are from. We need to be braver, push the boat away from the shore we know and face the uncertain waters of working altogether differently. In my next blog I will explore some of the possible ways we could work differently. As clinicians we must, as many have stated this week, build bridges not walls. There is far too much division, suspicion and competition amongst us. (Here comes the swearing)…..I was in a conversation with a consultant colleague recently and he was relaying to me that another consultant referred to GPs as a “bunch of Fuck Wits”. In a separate conversation, one of my GP colleagues referred to consultants as a “bunch of arrogant Shits”. These kind of attitudes pervade the NHS and have created a culture of dishonour, distrust and division. Honestly! We’re better than this. How are we going to create the new workforce of the future that works across our currently artificial boundaries if we don’t teach them basic respect? This week a patient came to see me because he was dismayed at having to have seen a nurse at the hospital after suffering a significant condition and wanted to check that I, as a doctor, was happy with what he had been told. I could have laughed it off, but I wanted to stand up for my nursing colleague, who actually has far more expertise in this area of medicine than I do. The advice he had been given was perfect and completely in line with the best guidance available. We must not be afraid to challenge attitudes that are antiquated and out of place. More than ever, we need a culture of honour. A culture of honour is one in which we believe the best of each other, speak well of each other and appreciate our brilliantly necessary but differing gifts and expertise. We need to work out how we work effectively together for the best of the people we serve. We need to connect with each other and rehumanise the system in which we work. When was the last time you met as a cross cultural or multidisciplinary team and simply told each other what you love and appreciate about each other and the work you do? If we can’t learn to be more relationally whole, we will continue to work in the midst of serious dysfunction and strife. Come on – amongst us we have some remarkable gifts of wisdom, healing and hope. Let’s build the kind of culture and community amongst us that stands shoulder to shoulder, changes the story in the media and speaks with one voice to the powers that we are about the a new way of working together through relationship not hierarchy and fear. What might we really achieve together? It is this kind of collaborative clinical community that can change the future of healthcare, not just in the UK, but right across the globe.
As clinicians we must, as many have stated this week, build bridges not walls. There is far too much division, suspicion and competition amongst us. (Here comes the swearing)…..I was in a conversation with a consultant colleague recently and he was relaying to me that another consultant referred to GPs as a “bunch of Fuck Wits”. In a separate conversation, one of my GP colleagues referred to consultants as a “bunch of arrogant Shits”. These kind of attitudes pervade the NHS and have created a culture of dishonour, distrust and division. Honestly! We’re better than this. How are we going to create the new workforce of the future that works across our currently artificial boundaries if we don’t teach them basic respect? This week a patient came to see me because he was dismayed at having to have seen a nurse at the hospital after suffering a significant condition and wanted to check that I, as a doctor, was happy with what he had been told. I could have laughed it off, but I wanted to stand up for my nursing colleague, who actually has far more expertise in this area of medicine than I do. The advice he had been given was perfect and completely in line with the best guidance available. We must not be afraid to challenge attitudes that are antiquated and out of place. More than ever, we need a culture of honour. A culture of honour is one in which we believe the best of each other, speak well of each other and appreciate our brilliantly necessary but differing gifts and expertise. We need to work out how we work effectively together for the best of the people we serve. We need to connect with each other and rehumanise the system in which we work. When was the last time you met as a cross cultural or multidisciplinary team and simply told each other what you love and appreciate about each other and the work you do? If we can’t learn to be more relationally whole, we will continue to work in the midst of serious dysfunction and strife. Come on – amongst us we have some remarkable gifts of wisdom, healing and hope. Let’s build the kind of culture and community amongst us that stands shoulder to shoulder, changes the story in the media and speaks with one voice to the powers that we are about the a new way of working together through relationship not hierarchy and fear. What might we really achieve together? It is this kind of collaborative clinical community that can change the future of healthcare, not just in the UK, but right across the globe.