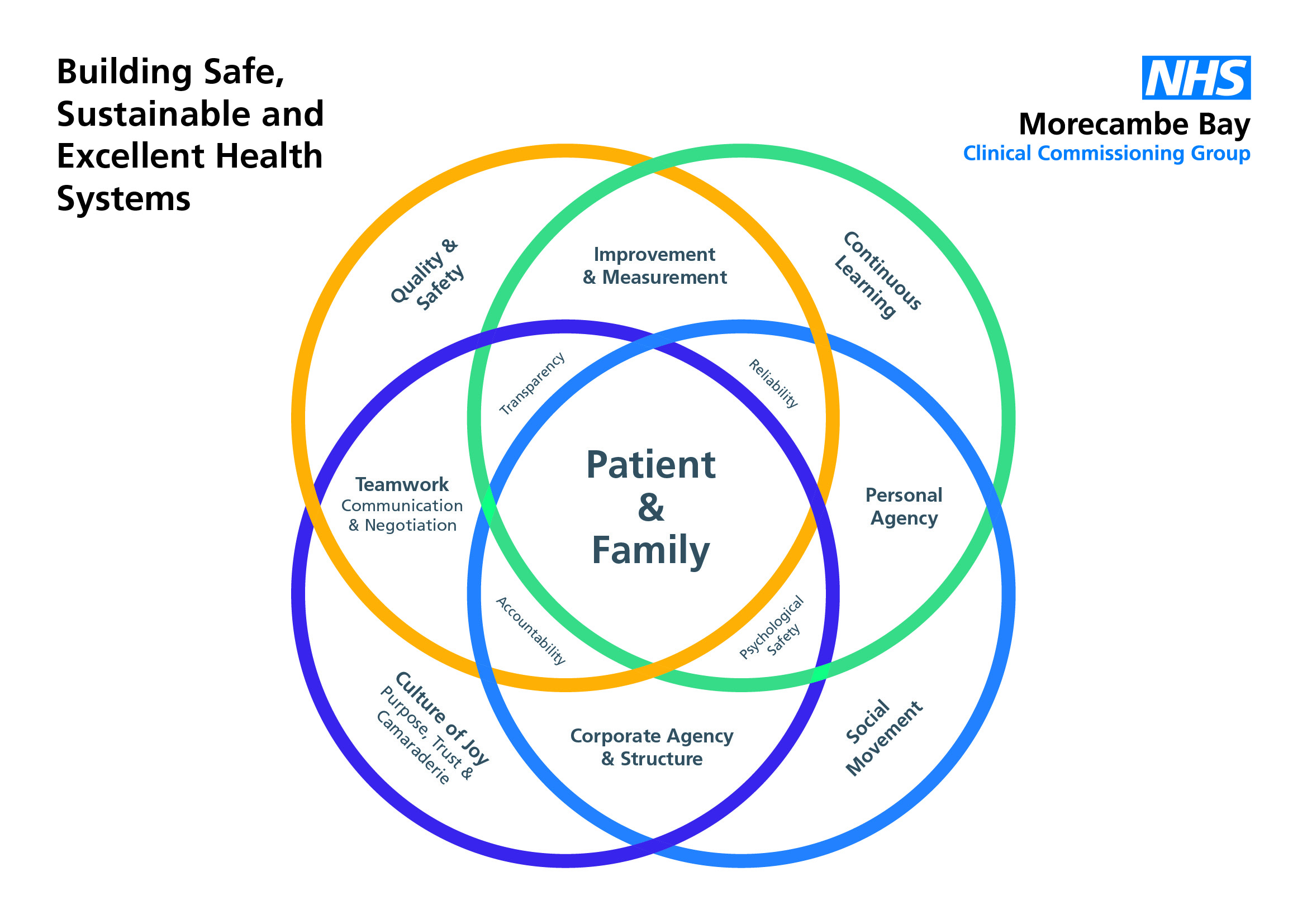
Learning requires humility. It requires us to accept that we don’t know everything, that we get it wrong sometimes, make mistakes and need to own up to them so that we don’t do the same thing again. Learning is a vital part of all we do in health and social care, if we are to create truly safe, sustainable, compassionate and excellent services. But humility, although vital, is not enough on its own. There are things we need to put in place to ensure our organisations are continually learning, and not only so but that we actually implement our learning and incorporating it into new ways of working so that we change as a result.
The IHI and Allan Frankel have come up with a really helpful and pretty straight forward framework which enables us to do this. It requires 3 basic ingredients:
1) Leadership commitment
2) Individual responsibility
3) A shared learning culture for quality and safety
Leadership is absolutely vital in setting the right structures and support in place for learning to take place. It requires:
-transparency with the public, patients and staff
-vulnerability about weaknesses
-openness about what is being learned and what is changing as a result
-ensuring we are learning with and from our patients not just within our clinically teams. (Some of the most powerful learning we have done in Morecambe Bay has been from women using our maternity services. Our attitudes, communication skills and expertise have all improved dramatically as a result).
-commitment to the psychological safety of staff in developing a culture in which no question is too stupid and no concern is dismissed
-genuine care for each member of staff, creating a culture in which every person can be mentored, coached and encouraged
-time given and protected in which learning can be fostered
Personal Responsibility
Who are you?
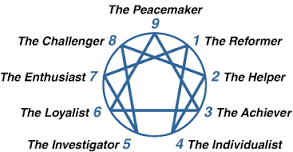 In my role as a coach/mentor or trainer I have found that we have become far too obsessed with ensuring that people have the right skills but not necessarily paying too much attention to who people are, what their character is like, what their strengths and weaknesses are and how they are developing as a human being. Our medical/nursing and other clinical schools are filled with people eager to learn but who often have no idea about who they are and who, not what they would like to become. Knowing who you are as a person, hugely affects your clinical practice and we do not give it any way near enough attention. I am personally a huge fan of the Enneagram. For me it has been transformational to understand as a type 7, not only what my root need is (to avoid pain) what my root struggle is (gluttony) how I do under stress (become a falsely happy control freak) but also, what my invitation is (towards sober joy and deeper understanding), how to become a more healthy version of me and therefore a better gift to my family, my team and all the people I’m trying to serve. It has helped me to recognise when I’m doing well and when I’m not and to understand how to bring my core strengths to the fore whilst also recognising where I need discipline and boundaries to function from a more healed place. We each have a responsibility not just to be good at stuff, but to be good at being us. And being us is more than just knowing how we function (e.g. ENFP in Myers-Briggs) but to get below the surface to the core of what makes us tick, that makes us human. Knowing who we truly are enables us to be better, kinder, more humble, genuine, compassionate people, who put aside the need to beat others down and learn to appreciate them so much more. When you really know the team you are working with, they become your friends, you understand the little idiosyncratic things about them with a whole lot more patience and you can also challenge them when they are not behaving in a way that is conducive to good care and you can also receive that challenge back when you are out of line. I wish that we were more interested in caring about who we are rather than only in what we can do. This has got to be a part of the culture of joy I have blogged about previously.
In my role as a coach/mentor or trainer I have found that we have become far too obsessed with ensuring that people have the right skills but not necessarily paying too much attention to who people are, what their character is like, what their strengths and weaknesses are and how they are developing as a human being. Our medical/nursing and other clinical schools are filled with people eager to learn but who often have no idea about who they are and who, not what they would like to become. Knowing who you are as a person, hugely affects your clinical practice and we do not give it any way near enough attention. I am personally a huge fan of the Enneagram. For me it has been transformational to understand as a type 7, not only what my root need is (to avoid pain) what my root struggle is (gluttony) how I do under stress (become a falsely happy control freak) but also, what my invitation is (towards sober joy and deeper understanding), how to become a more healthy version of me and therefore a better gift to my family, my team and all the people I’m trying to serve. It has helped me to recognise when I’m doing well and when I’m not and to understand how to bring my core strengths to the fore whilst also recognising where I need discipline and boundaries to function from a more healed place. We each have a responsibility not just to be good at stuff, but to be good at being us. And being us is more than just knowing how we function (e.g. ENFP in Myers-Briggs) but to get below the surface to the core of what makes us tick, that makes us human. Knowing who we truly are enables us to be better, kinder, more humble, genuine, compassionate people, who put aside the need to beat others down and learn to appreciate them so much more. When you really know the team you are working with, they become your friends, you understand the little idiosyncratic things about them with a whole lot more patience and you can also challenge them when they are not behaving in a way that is conducive to good care and you can also receive that challenge back when you are out of line. I wish that we were more interested in caring about who we are rather than only in what we can do. This has got to be a part of the culture of joy I have blogged about previously.
How are you?
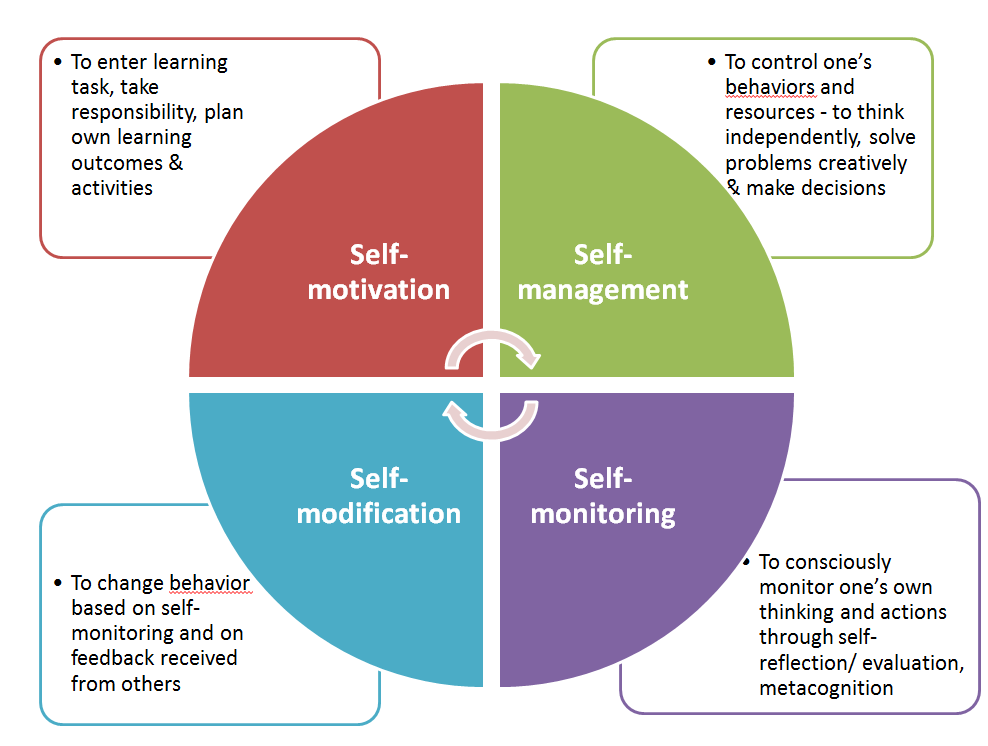 Personal responsibility beckons us to be more honest with ourselves and others about how we’re doing emotionally/physically/mentally. It has been a transformational practice in our team to simply check-in with each other and talk about where we’re at. In this way, we can carry each other when needed and treat each other with kindness and compassion. But our individual agency, must also cause us to recognise when we are at a wall/ceiling/limit personally or professionally. We must simply own up when we don’t know something or are out of our depth or need help. We cannot pretend to be able to have a competency that we don’t have. We need to be self-aware and humble enough to accept when we don’t know something or have become unwell and ensure that we take it upon ourselves to find out or get the help we need. This is learning to have an internal, rather than an external locus of control. An external locus, always looks elsewhere for the answer. An internal
Personal responsibility beckons us to be more honest with ourselves and others about how we’re doing emotionally/physically/mentally. It has been a transformational practice in our team to simply check-in with each other and talk about where we’re at. In this way, we can carry each other when needed and treat each other with kindness and compassion. But our individual agency, must also cause us to recognise when we are at a wall/ceiling/limit personally or professionally. We must simply own up when we don’t know something or are out of our depth or need help. We cannot pretend to be able to have a competency that we don’t have. We need to be self-aware and humble enough to accept when we don’t know something or have become unwell and ensure that we take it upon ourselves to find out or get the help we need. This is learning to have an internal, rather than an external locus of control. An external locus, always looks elsewhere for the answer. An internal 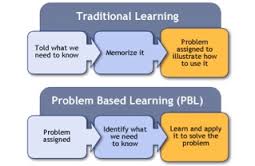 locus takes responsibility to find out and keep learning. We need to develop a core value, that learning is really really important and we will prioritise ensuring that we keep making time to do so, through whatever form that takes, especially reflective practice. Yes there is some dependency on supportive structures and time being given, but there is also that sense of motivation that comes from within that we take ourselves and our roles seriously. It’s one of the reasons why I’m such a fan of a combination of problem-based learning and a solutions-focussed approach. If we do this ourselves and foster it in our teams, the care we provide will be beyond stellar!
locus takes responsibility to find out and keep learning. We need to develop a core value, that learning is really really important and we will prioritise ensuring that we keep making time to do so, through whatever form that takes, especially reflective practice. Yes there is some dependency on supportive structures and time being given, but there is also that sense of motivation that comes from within that we take ourselves and our roles seriously. It’s one of the reasons why I’m such a fan of a combination of problem-based learning and a solutions-focussed approach. If we do this ourselves and foster it in our teams, the care we provide will be beyond stellar!
Why are you Here?
We talk about the law of two feet in our team. You are responsible to know why you are here, or if you need to be somewhere else. That might even mean a job change, but more often than not it means having some good boundaries, knowing whether or not you really need to be at a certain meeting or somewhere else, if you should be doing what you are or if you need to ensure other things get the right focus. And what about yourself? Have you taken time to eat well, stay well hydrated, exercise, sleep well, maintain health in your relationships? In teams that care for each other we need to help each other to know why we are there and why we are important.
A Shared Learning Culture
 It’s amazing to me that so many of our learning environments are still so teacher-based. Adult education is so much more empowering than this and it’s high time our clinical learning environments (both preclinical and in every day life) reflect this. They should also be more inclusive and we should be learning with and from our patients far more than we do. Although the above graphic applies to classroom settings, it contains many lessons for us.
It’s amazing to me that so many of our learning environments are still so teacher-based. Adult education is so much more empowering than this and it’s high time our clinical learning environments (both preclinical and in every day life) reflect this. They should also be more inclusive and we should be learning with and from our patients far more than we do. Although the above graphic applies to classroom settings, it contains many lessons for us.
With leadership and personal agency holding true, a culture then develops in which continuous learning is the norm. Learning environments, fuelled by kenotic power create a space in which an organisation can begin to truly flourish. It creates a net of accountability, teamwork, improvement and measurement, making the entire system more reliable. It is vital that we create this as one of the core principles upon which we build our future health and social care systems.


























 All this week on the BBC, there has been a focus on the NHS and the crisis we are in – don’t panic Mr Mainwaring…..There is a heady mix of opinions being thrown around – Question Time became quite a furore of ideas and thoughts last night – not enough beds, not enough staff, not enough money, too much money, too many patients, too many wasted appointments, too many malingerers, too many ill people, too many old people, too many managers, too many drugs, too many drunkards, disappointed clinicians, disappointed patients, disappointed MPs, a disappointed health secretary – what are we to think and what are we to do?
All this week on the BBC, there has been a focus on the NHS and the crisis we are in – don’t panic Mr Mainwaring…..There is a heady mix of opinions being thrown around – Question Time became quite a furore of ideas and thoughts last night – not enough beds, not enough staff, not enough money, too much money, too many patients, too many wasted appointments, too many malingerers, too many ill people, too many old people, too many managers, too many drugs, too many drunkards, disappointed clinicians, disappointed patients, disappointed MPs, a disappointed health secretary – what are we to think and what are we to do? We love the NHS because it speaks something to us about our togetherness and our commitment to health justice for all. This circular argument about money is the wrong conversation and it is beginning to have a very nasty undertone about who we might be able to blame and scapegoat in order to solve the mess we are in. Let’s be very clear. The NHS is NOT in crisis because of refugees, asylum seekers, immigrants or health tourists. I’m going to stick my neck out here – it isn’t even the fault of the current and previous health secretaries, though it would be easy to play the blame game that way too. The NHS is in crisis, because the entire Western World is in crisis! Our economic systems are broken and our political systems are pretty defunct. We have built our nation state on the foundations of empire. We have built our economy on conquest and slavery and have used debt, violence and law to keep control….but everything is shaking.
We love the NHS because it speaks something to us about our togetherness and our commitment to health justice for all. This circular argument about money is the wrong conversation and it is beginning to have a very nasty undertone about who we might be able to blame and scapegoat in order to solve the mess we are in. Let’s be very clear. The NHS is NOT in crisis because of refugees, asylum seekers, immigrants or health tourists. I’m going to stick my neck out here – it isn’t even the fault of the current and previous health secretaries, though it would be easy to play the blame game that way too. The NHS is in crisis, because the entire Western World is in crisis! Our economic systems are broken and our political systems are pretty defunct. We have built our nation state on the foundations of empire. We have built our economy on conquest and slavery and have used debt, violence and law to keep control….but everything is shaking. brave enough to rewire our brains, realign our values and reimagine a different way of being together? If we accept that things simply cannot remain as they are, might we instead find one another in fresh ways and discover new ways of being in which we’re not always chasing the money, with all its strings attached, but choosing something altogether more life giving?
brave enough to rewire our brains, realign our values and reimagine a different way of being together? If we accept that things simply cannot remain as they are, might we instead find one another in fresh ways and discover new ways of being in which we’re not always chasing the money, with all its strings attached, but choosing something altogether more life giving? I would suggest we need two things (an ambidextrous approach) – both of which are already happening, we just need to recognise them, fan the flames and watch the new emerge, whilst Rome burns around us.
I would suggest we need two things (an ambidextrous approach) – both of which are already happening, we just need to recognise them, fan the flames and watch the new emerge, whilst Rome burns around us. are beginning to think about how we are living and making a change. It’s a tough reality, but there is personal and corporate responsibility that we need to take. We cannot keep shoving poison into our bodies or treating them badly and expect that we will be well, or that we will be able to afford the drugs to fix us. Social movements are beginning to emerge and we need to be a part of them. Together, we can! Together we can cause corporations to change their behaviour and act in accordance with what is right, true, just, kind and loving. We can also choose to take responsibility for what we buy and how much exercise we do. Here in Morecambe Bay we are launching the Morecambe Bay Mile, encouraging everyone to move a mile a day without transport! We’re also working with our communities around diet. We’re also connecting with amazing people doing amazing things and seeing just how much kindness and goodness there is in the communities around us. Our happiness is directly linked to the quality and depth of our friendships. People being together and facing up to the issues together is absolutely key to our long term health.
are beginning to think about how we are living and making a change. It’s a tough reality, but there is personal and corporate responsibility that we need to take. We cannot keep shoving poison into our bodies or treating them badly and expect that we will be well, or that we will be able to afford the drugs to fix us. Social movements are beginning to emerge and we need to be a part of them. Together, we can! Together we can cause corporations to change their behaviour and act in accordance with what is right, true, just, kind and loving. We can also choose to take responsibility for what we buy and how much exercise we do. Here in Morecambe Bay we are launching the Morecambe Bay Mile, encouraging everyone to move a mile a day without transport! We’re also working with our communities around diet. We’re also connecting with amazing people doing amazing things and seeing just how much kindness and goodness there is in the communities around us. Our happiness is directly linked to the quality and depth of our friendships. People being together and facing up to the issues together is absolutely key to our long term health. Secondly, we must stop serving the system, re-humanise it, call it in line and cause it to serve the needs of the people and the planet (the right handed approach). Those in the health and social care system must refuse to be bullied by the powers into ways of behaving, stop thinking they have the answers and therefore coming up with another new scheme to do to people and be willing to listen to and work with the emerging social movements. This will allow us to see a society that is much more well and therefore in need of less care. But where care is needed, we have to accept that we have allowed ourselves to be competitive rather than collaborative, hierarchical instead of co-operative and our own attitudes and behaviours are stopping us from giving the compassionate care we long to deliver. We cannot make excuses. We must let go of self-protectionism. We must be willing to change the way we think and behave, breaking down walls, letting go of suspicion and cutting through red tape so that we provide the care which we can. This is happening, here in Morecambe Bay – but it’s not a quick thing. We are rediscovering the power of relationship and daring to make some bold steps into delivering care very differently – but for those of you outside the system, please understand, it takes time and feels pretty scary!
Secondly, we must stop serving the system, re-humanise it, call it in line and cause it to serve the needs of the people and the planet (the right handed approach). Those in the health and social care system must refuse to be bullied by the powers into ways of behaving, stop thinking they have the answers and therefore coming up with another new scheme to do to people and be willing to listen to and work with the emerging social movements. This will allow us to see a society that is much more well and therefore in need of less care. But where care is needed, we have to accept that we have allowed ourselves to be competitive rather than collaborative, hierarchical instead of co-operative and our own attitudes and behaviours are stopping us from giving the compassionate care we long to deliver. We cannot make excuses. We must let go of self-protectionism. We must be willing to change the way we think and behave, breaking down walls, letting go of suspicion and cutting through red tape so that we provide the care which we can. This is happening, here in Morecambe Bay – but it’s not a quick thing. We are rediscovering the power of relationship and daring to make some bold steps into delivering care very differently – but for those of you outside the system, please understand, it takes time and feels pretty scary! more healthy and well and we changed our ways of working to be more collaborative and kind. It is this ambidextrous approach to health and wellbeing, in which a heady mix of an invigorated people movement and a reorientated system working together for the good of everyone everywhere, might breathe hope into other parts of the world that out of the old can come something new. Maybe it is just possible that healthcare can be provided for everyone everywhere when people are brave enough to let go of old ways, embrace the brokenness of our reality and find a new way through together.
more healthy and well and we changed our ways of working to be more collaborative and kind. It is this ambidextrous approach to health and wellbeing, in which a heady mix of an invigorated people movement and a reorientated system working together for the good of everyone everywhere, might breathe hope into other parts of the world that out of the old can come something new. Maybe it is just possible that healthcare can be provided for everyone everywhere when people are brave enough to let go of old ways, embrace the brokenness of our reality and find a new way through together. I’m telling you – it is nearly Spring time and the bulbs are beginning to break through. Can you smell the scent of something new emerging? Those rhizomal roots of the snowdrops – that interconnected underground network that shoots up its flowers, is telling us the winter of discontent is over. It’s time to turn off the radio, dial down the meta narrative of fear and instead, put on love, hope and faith, find each other, change our ways of working and step into the future we know our hearts yearn for.
I’m telling you – it is nearly Spring time and the bulbs are beginning to break through. Can you smell the scent of something new emerging? Those rhizomal roots of the snowdrops – that interconnected underground network that shoots up its flowers, is telling us the winter of discontent is over. It’s time to turn off the radio, dial down the meta narrative of fear and instead, put on love, hope and faith, find each other, change our ways of working and step into the future we know our hearts yearn for.